Open-angle glaucoma: Difference between revisions
| (5 intermediate revisions by the same user not shown) | |||
| Line 8: | Line 8: | ||
**Increased aqueous production | **Increased aqueous production | ||
**Decreased outflow | **Decreased outflow | ||
===Etiologies<ref>Optometric Clinical Practice Guideline Care of the Patient with Open Angle Glaucoma. Fingeret, M. American Optometric Association Original Consensus Panel on Care of the Patient with Open Angle Glaucoma. American Optometric Association, 2011</ref>=== | |||
*Primary | |||
*Secondary | |||
**Another ocular disease | |||
**Systemic disease | |||
**Trauma | |||
**Drugs | |||
==Clinical Features== | ==Clinical Features== | ||
| Line 19: | Line 27: | ||
==Evaluation== | ==Evaluation== | ||
===Workup=== | ===Workup=== | ||
*[[Eye exam]] with IOP check | |||
===Diagnosis=== | ===Diagnosis=== | ||
*Characteristic nerve damage (eg, cupping) on fundus examination | *Characteristic nerve damage (eg, cupping) on fundus examination | ||
*Visual field abnormalities | *Visual field abnormalities | ||
*+/- elevated IOP | *+/- elevated IOP (>21 mmHg) | ||
==Management== | ==Management== | ||
*Typically managed chronically with long-term eye drops or outpatient procedures and does not | *Typically managed chronically with long-term eye drops or outpatient procedures and does not typically requir immediate emergency intervention | ||
==Disposition== | ==Disposition== | ||
Latest revision as of 23:16, 4 February 2026
Background
- Elevated intraocular pressure and resulting optic nerve damage manifested initially as visual field loss and ultimately irreversible blindness if left untreated
- Unclear pathogenesis, however thought to be related to two mechanisms:
- Increased aqueous production
- Decreased outflow
Etiologies[1]
- Primary
- Secondary
- Another ocular disease
- Systemic disease
- Trauma
- Drugs
Clinical Features
- Rarely experience symptoms, in contrast to acute angle closure glaucoma
- Typical pattern characterized by progressive peripheral visual field loss followed by central field loss, usually but not always associated with elevated intraocular pressure
Differential Diagnosis
Acute Vision Loss (Noninflamed)
- Painful
- Arteritic anterior ischemic optic neuropathy
- Optic neuritis
- Temporal arteritis†
- Painless
- Amaurosis fugax
- Central retinal artery occlusion (CRAO)†
- Central retinal vein occlusion (CRVO)†
- High altitude retinopathy
- Open-angle glaucoma
- Posterior reversible encephalopathy syndrome (PRES)
- Retinal detachment†
- Stroke†
- Vitreous hemorrhage
- Traumatic optic neuropathy (although may have pain from the trauma)
†Emergent Diagnosis
Evaluation
Workup
- Eye exam with IOP check
Diagnosis
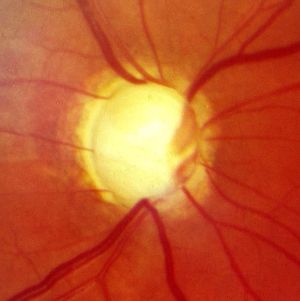
- Characteristic nerve damage (eg, cupping) on fundus examination
- Visual field abnormalities
- +/- elevated IOP (>21 mmHg)
Management
- Typically managed chronically with long-term eye drops or outpatient procedures and does not typically requir immediate emergency intervention
Disposition
- Outpatient
See Also
External Links
References
- ↑ Optometric Clinical Practice Guideline Care of the Patient with Open Angle Glaucoma. Fingeret, M. American Optometric Association Original Consensus Panel on Care of the Patient with Open Angle Glaucoma. American Optometric Association, 2011