Polymorphic ventricular tachycardia: Difference between revisions
Neil.m.young (talk | contribs) (Text replacement - "EKG" to "ECG") |
(Add verified PubMed references (PMIDs 34491774, 37558300)) |
||
| (25 intermediate revisions by 8 users not shown) | |||
| Line 1: | Line 1: | ||
==Background== | ==Background== | ||
*Form of [[ventricular tachycardia]] | *Form of [[ventricular tachycardia]]<ref>Viskin S, et al. Polymorphic Ventricular Tachycardia: Terminology, Mechanism, Diagnosis, and Emergency Therapy. Circulation. 2021 Sep 7;144(10):823-839. PMID 34491774</ref> | ||
*Subtypes include [[Torsades de pointes]], bidirectional polymorphic VTach (seen in [[digoxin toxicity]] | **Multiple ventricular foci | ||
**QRS complexes with varying morphology | |||
*Subtypes include: | |||
**[[Torsades de pointes]]<ref>Bergeman AT, Wilde AAM, van der Werf C. Catecholaminergic Polymorphic Ventricular Tachycardia: A Review of Therapeutic Strategies. Card Electrophysiol Clin. 2023 Sep;15(3):293-305. PMID 37558300</ref> | |||
**bidirectional polymorphic [[VTach]] (as seen in [[digoxin toxicity]]) | |||
===Etiologies=== | ===Etiologies=== | ||
| Line 15: | Line 19: | ||
*[[Syncope]] | *[[Syncope]] | ||
*[[Palpitations]] | *[[Palpitations]] | ||
*[[Altered level of consciousness]] | |||
* | *May present with [[cardiac arrest]] | ||
* | |||
==Differential Diagnosis== | ==Differential Diagnosis== | ||
{{Tachycardia (wide) DDX}} | |||
==Evaluation== | ==Evaluation== | ||
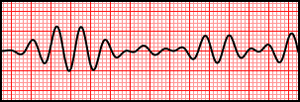
[[File:Torsades de Pointes (polymorphic VT).svg|thumb|Torsades de Pointes in a rhythm strip.]] | |||
*Evaluate for underlying causes (e.g. electrolyte imbalances, [[ACS]]) | *Evaluate for underlying causes (e.g. electrolyte imbalances, [[ACS]]) | ||
===[[ECG]] Findings=== | |||
*Wide QRS (>100ms or 3 small boxes) | |||
*QRS complexes of varied amplitude, axis and duration | |||
**Torsades: QRS complexes appear to twist around isoelectric line | |||
*Rapid rhythm (usually 140-160 bpm, but can be up to 300 bpm) | |||
*Irregular | |||
==Management== | ==Management== | ||
| Line 40: | Line 44: | ||
===Stable=== | ===Stable=== | ||
*Correct any electrolyte abnormalities | *Correct any electrolyte abnormalities | ||
*Torsades: | *[[Torsades]]: | ||
**[[Magnesium]] sulfate (for Torsades): | **[[Magnesium]] sulfate (for Torsades): | ||
***1-2gm IV, repeat in 5-15min; then 1-2gm/hr (3-10mg/min) drip | ***1-2gm IV, repeat in 5-15min; then 1-2gm/hr (3-10mg/min) drip | ||
***Peds: 25-50mg/kg (max 2g) IV | ***Peds: 25-50mg/kg (max 2g) IV | ||
**[[Isoproterenol]], 2-8 mcg/min (if available) | |||
**[[Isoproterenol]], 2-8 mcg/min | **[[Overdrive Pacing]] to goal HR 90-120 | ||
**[[Overdrive Pacing]] to goal HR 90-120 | ***Note that this is only effective for preventing recurrence of TdP - it will not convert TdP to sinus rhythm | ||
**Consider Lidocaine | |||
**Avoid procainamide, amiodarone (may further prolong QT) | **Avoid procainamide, amiodarone (may further prolong QT) | ||
*Non-Torsades | *Non-Torsades (baseline QT interval not prolonged) | ||
**[[Amiodarone]], agent of choice in setting of AMI or LV dysfunction | **[[Amiodarone]], agent of choice in setting of AMI or LV dysfunction | ||
***150 mg over 10min (15 mg/min), followed by 1 mg/min drip over 6hrs (360 mg total), then 0.5 mg/min drip over next 18 hrs (540 mg total) | ***150 mg over 10min (15 mg/min), followed by 1 mg/min drip over 6hrs (360 mg total), then 0.5 mg/min drip over next 18 hrs (540 mg total) | ||
| Line 54: | Line 59: | ||
**[[Procainamide]] | **[[Procainamide]] | ||
***100 mg q5min until termination of arrhythmia, then start 2-6 mg/min (or 1-2 mg/min for renal/cardiac failure) | ***100 mg q5min until termination of arrhythmia, then start 2-6 mg/min (or 1-2 mg/min for renal/cardiac failure) | ||
***Max dose 17mg/kg OR widening of QRS >50% | ***Max dose 17mg/kg '''OR''' widening of QRS >50% | ||
**[[Lidocaine]], 1-1.5mg/kg IV q5min, repeat | **[[Lidocaine]], 1-1.5mg/kg IV q5min, repeat PRN up to 300mg/hr | ||
**[[Beta-blockers]] (e.g. [[metoprolol]] 5mg IV q5m x 3) if blood pressure tolerates | |||
===Refractory=== | ===Refractory=== | ||
*≥3 episodes within 24 hours considered [[electrical storm]] | *≥3 episodes within 24 hours considered [[electrical storm]] | ||
*May require alternate treatment (i.e. [[ | *May require alternate treatment (i.e. [[β-blockers]], sedation, ablation) | ||
==Medication Dosing== | |||
{{MedicationDose | |||
| drug = Magnesium sulfate | |||
| dose = 1-2g IV, repeat in 5-15min; then 1-2g/hr infusion | |||
| route = IV | |||
| context = Torsades de pointes | |||
| indication = Polymorphic ventricular tachycardia | |||
| population = Adult | |||
}} | |||
{{MedicationDose | |||
| drug = Magnesium sulfate | |||
| dose = 25-50mg/kg (max 2g) IV | |||
| route = IV | |||
| context = Torsades de pointes | |||
| indication = Polymorphic ventricular tachycardia | |||
| population = Pediatric | |||
}} | |||
{{MedicationDose | |||
| drug = Isoproterenol | |||
| dose = 2-8mcg/min IV infusion | |||
| route = IV | |||
| context = Torsades de pointes | |||
| indication = Polymorphic ventricular tachycardia | |||
| population = Adult | |||
}} | |||
{{MedicationDose | |||
| drug = Amiodarone | |||
| dose = 150mg IV over 10min, then 1mg/min x6hr, then 0.5mg/min x18hr | |||
| route = IV | |||
| context = Non-torsades PMVT, AMI or LV dysfunction | |||
| indication = Polymorphic ventricular tachycardia | |||
| population = Adult | |||
}} | |||
{{MedicationDose | |||
| drug = Amiodarone | |||
| dose = 5mg/kg (max 300mg) IV, may repeat x2 | |||
| route = IV | |||
| context = Non-torsades PMVT | |||
| indication = Polymorphic ventricular tachycardia | |||
| population = Pediatric | |||
}} | |||
{{MedicationDose | |||
| drug = Lidocaine | |||
| dose = 1-1.5mg/kg IV, then 1-4mg/min infusion | |||
| route = IV | |||
| context = Non-torsades PMVT, alternative agent | |||
| indication = Polymorphic ventricular tachycardia | |||
| population = Adult | |||
}} | |||
{{MedicationDose | |||
| drug = Lidocaine | |||
| dose = 1mg/kg (max 100mg) IV | |||
| route = IV | |||
| context = Non-torsades PMVT | |||
| indication = Polymorphic ventricular tachycardia | |||
| population = Pediatric | |||
}} | |||
{{MedicationDose | |||
| drug = Procainamide | |||
| dose = 20-50mg/min IV (max 17mg/kg) | |||
| route = IV | |||
| context = Non-torsades PMVT, baseline QT not prolonged | |||
| indication = Polymorphic ventricular tachycardia | |||
| population = Adult | |||
}} | |||
{{MedicationDose | |||
| drug = Procainamide | |||
| dose = 15mg/kg IV over 30-60min | |||
| route = IV | |||
| context = Non-torsades PMVT | |||
| indication = Polymorphic ventricular tachycardia | |||
| population = Pediatric | |||
}} | |||
==Disposition== | ==Disposition== | ||
*Admit, even if back in normal sinus rhythm | *Admit with cardiology consult, even if back in normal sinus rhythm | ||
**Stable patients may be admitted to ward | |||
***Pads should remain on patient's chest anticipating need for repeat cardioversion | |||
***All patients should remain on telemetry or full cardio-respiratory monitoring for recurrent events | |||
**Patients with features of instability or refractory VT are best admitted to CCU or ICU and may require urgent or emergent pacemaker placement | |||
==See Also== | ==See Also== | ||
| Line 70: | Line 154: | ||
*[[Adult Pulseless Arrest]], [[Pediatric pulseless arrest]] | *[[Adult Pulseless Arrest]], [[Pediatric pulseless arrest]] | ||
*[[Critical care quick reference]] | *[[Critical care quick reference]] | ||
*[[Nonsustained ventricular tachycardia]] | |||
==External Links== | ==External Links== | ||
Latest revision as of 10:43, 22 March 2026
Background
- Form of ventricular tachycardia[1]
- Multiple ventricular foci
- QRS complexes with varying morphology
- Subtypes include:
- Torsades de pointes[2]
- bidirectional polymorphic VTach (as seen in digoxin toxicity)
Etiologies
- Myocardial ischemia (most common)
- Acquired or congenital prolonged QT
- TCAs, phenothiazines, Type I antiarrhythmics (quinidine, procainamide)
- Hypokalemia
- Hypomagnesemia
- Elevated intracranial pressure
- Brugada syndrome, short QT syndrome, congenital catecholaminergic polymorphic ventricular tachycardia
Clinical Features
- Syncope
- Palpitations
- Altered level of consciousness
- May present with cardiac arrest
Differential Diagnosis
Wide-complex tachycardia
Assume any wide-complex tachycardia is ventricular tachycardia until proven otherwise (it is safer to incorrectly assume a ventricular dysrhythmia than supraventricular tachycardia with abberancy)
- Regular
- Monomorphic ventricular tachycardia
- PSVT with aberrant conduction:
- PSVT with bundle branch block^
- PSVT with accessory pathway
- Atrial flutter with bundle branch block^
- Sinus tachycardia with bundle branch block^
- Accelerated idioventricular rhythm (consider if less than or ~120 bpm)
- Metabolic
- Irregular
- Atrial fibrillation/atrial flutter with variable AV conduction AND bundle branch block^
- Atrial fibrillation/atrial flutter with variable AV conduction AND accessory pathway (e.g. WPW)
- Atrial fibrillation + hyperkalemia
- Polymorphic ventricular tachycardia
^Fixed or rate-related
Evaluation
- Evaluate for underlying causes (e.g. electrolyte imbalances, ACS)
ECG Findings
- Wide QRS (>100ms or 3 small boxes)
- QRS complexes of varied amplitude, axis and duration
- Torsades: QRS complexes appear to twist around isoelectric line
- Rapid rhythm (usually 140-160 bpm, but can be up to 300 bpm)
- Irregular
Management
Pulseless
See Adult pulseless arrest and Pediatric pulseless arrest
Unstable
- Unsynchronized cardioversion (defibrillation) 200J (or 2J/kg for pediatrics)
- Correct any electrolyte abnormalities
Stable
- Correct any electrolyte abnormalities
- Torsades:
- Magnesium sulfate (for Torsades):
- 1-2gm IV, repeat in 5-15min; then 1-2gm/hr (3-10mg/min) drip
- Peds: 25-50mg/kg (max 2g) IV
- Isoproterenol, 2-8 mcg/min (if available)
- Overdrive Pacing to goal HR 90-120
- Note that this is only effective for preventing recurrence of TdP - it will not convert TdP to sinus rhythm
- Consider Lidocaine
- Avoid procainamide, amiodarone (may further prolong QT)
- Magnesium sulfate (for Torsades):
- Non-Torsades (baseline QT interval not prolonged)
- Amiodarone, agent of choice in setting of AMI or LV dysfunction
- 150 mg over 10min (15 mg/min), followed by 1 mg/min drip over 6hrs (360 mg total), then 0.5 mg/min drip over next 18 hrs (540 mg total)
- Peds: 5mg/kg (max 300mg), may repeat twice
- Procainamide
- 100 mg q5min until termination of arrhythmia, then start 2-6 mg/min (or 1-2 mg/min for renal/cardiac failure)
- Max dose 17mg/kg OR widening of QRS >50%
- Lidocaine, 1-1.5mg/kg IV q5min, repeat PRN up to 300mg/hr
- Beta-blockers (e.g. metoprolol 5mg IV q5m x 3) if blood pressure tolerates
- Amiodarone, agent of choice in setting of AMI or LV dysfunction
Refractory
- ≥3 episodes within 24 hours considered electrical storm
- May require alternate treatment (i.e. β-blockers, sedation, ablation)
Medication Dosing
Magnesium sulfate 1-2g IV, repeat in 5-15min; then 1-2g/hr infusion IV Magnesium sulfate 25-50mg/kg (max 2g) IV IV Isoproterenol 2-8mcg/min IV infusion IV Amiodarone 150mg IV over 10min, then 1mg/min x6hr, then 0.5mg/min x18hr IV Amiodarone 5mg/kg (max 300mg) IV, may repeat x2 IV Lidocaine 1-1.5mg/kg IV, then 1-4mg/min infusion IV Lidocaine 1mg/kg (max 100mg) IV IV Procainamide 20-50mg/min IV (max 17mg/kg) IV Procainamide 15mg/kg IV over 30-60min IV
Disposition
- Admit with cardiology consult, even if back in normal sinus rhythm
- Stable patients may be admitted to ward
- Pads should remain on patient's chest anticipating need for repeat cardioversion
- All patients should remain on telemetry or full cardio-respiratory monitoring for recurrent events
- Patients with features of instability or refractory VT are best admitted to CCU or ICU and may require urgent or emergent pacemaker placement
- Stable patients may be admitted to ward
See Also
- Tachycardia (wide)
- Torsades de pointes
- ACLS (Main), PALS (Main)
- Adult Pulseless Arrest, Pediatric pulseless arrest
- Critical care quick reference
- Nonsustained ventricular tachycardia
External Links
References
- ↑ Viskin S, et al. Polymorphic Ventricular Tachycardia: Terminology, Mechanism, Diagnosis, and Emergency Therapy. Circulation. 2021 Sep 7;144(10):823-839. PMID 34491774
- ↑ Bergeman AT, Wilde AAM, van der Werf C. Catecholaminergic Polymorphic Ventricular Tachycardia: A Review of Therapeutic Strategies. Card Electrophysiol Clin. 2023 Sep;15(3):293-305. PMID 37558300