Arthritis: Difference between revisions
(Created page with "==DDX By Number of Affected Joints== #Monoarthritis ##Trauma-induced arthritis ##Nongonococcal septic arthritis ##Gonococcal septic arthritis ##Crystal-induced (gout, pseudogout)...") |
(Add verified PubMed reference (PMID 28366221)) |
||
| (37 intermediate revisions by 7 users not shown) | |||
| Line 1: | Line 1: | ||
== | ==Background== | ||
*Arthritis refers to joint inflammation, characterized by pain, swelling, warmth, and decreased range of motion<ref>Ross JJ. Septic Arthritis of Native Joints. Infect Dis Clin North Am. 2017 Jun;31(2):203-218. PMID 28366221</ref> | |||
*The primary EM concern is ruling out '''[[septic arthritis]]''', which is a joint emergency requiring urgent drainage | |||
*Classification by number of joints involved helps narrow the differential: | |||
**Monoarticular (1 joint): [[septic arthritis]], crystal disease, hemarthrosis — see [[Monoarticular arthritis]] | |||
**Oligoarticular (2-4 joints): reactive arthritis, seronegative spondyloarthropathy, gonococcal arthritis | |||
**Polyarticular (≥5 joints): rheumatoid arthritis, viral arthritis, SLE, rheumatic fever | |||
**Migratory: rheumatic fever, gonococcal arthritis, viral | |||
*Key distinction: inflammatory (warm, swollen, worse with rest, morning stiffness >30 min) vs. non-inflammatory/mechanical (worse with activity, minimal swelling, no morning stiffness) | |||
== | ==Clinical Features== | ||
===History=== | |||
*Number and pattern of joints involved | |||
*Acute vs. chronic onset | |||
*Symmetric vs. asymmetric distribution | |||
*Morning stiffness: >30-60 minutes suggests inflammatory arthritis | |||
*Recent infection: pharyngitis (post-strep/rheumatic fever), GI illness (reactive arthritis), STI (gonococcal) | |||
*Skin findings: rash, psoriasis, tophi, dermatitis-arthritis syndrome | |||
*Eye symptoms: conjunctivitis (reactive arthritis), uveitis (ankylosing spondylitis) | |||
*Trauma history | |||
*Family history of autoimmune disease | |||
*Medication history: diuretics, [[cyclosporine]] (gout risk) | |||
== | ===Physical Exam=== | ||
* | *Joint warmth, swelling, effusion, tenderness | ||
*Range of motion (active and passive) | |||
*Pain with passive ROM suggests intra-articular pathology | |||
*Periarticular tenderness without effusion suggests bursitis/tendinitis (periarticular, not articular) | |||
*Skin: tophi (gout), dactylitis (psoriatic arthritis), rash, nail pitting (psoriasis) | |||
*Mucocutaneous lesions (gonococcal — pustules on palms/soles, tenosynovitis) | |||
*Heart murmur (endocarditis, rheumatic fever) | |||
[[Category: | ===Red Flags=== | ||
*Hot, swollen, single joint = septic until proven otherwise → [[arthrocentesis]] | |||
*Fever with joint complaints (septic arthritis, endocarditis) | |||
*Prosthetic joint with new pain/swelling (prosthetic joint infection) | |||
*IV drug use + joint pain (hematogenous seeding) | |||
*Polyarthritis + new murmur (endocarditis) | |||
*Pediatric arthritis + fever + rash (consider [[Kawasaki disease]], [[rheumatic fever]], JIA) | |||
==Differential Diagnosis== | |||
{{Differential Diagnosis Monoarthritis}} | |||
{{Differntial Diagnosis Oligoarthritis}} | |||
{{Differential Diagnosis Polyarthritis}} | |||
{{Differencial Diagnosis Migratory Arthritis}} | |||
==Evaluation== | |||
===Monoarticular (Most Critical Workup)=== | |||
*[[Arthrocentesis]] — perform on any acute hot, swollen joint | |||
**Synovial fluid: cell count, Gram stain, culture, crystal analysis | |||
**WBC >50,000 with >90% PMNs = presumed septic until culture results | |||
**Crystals: negatively birefringent (gout), positively birefringent (pseudogout) | |||
**Note: crystals do NOT rule out co-existing infection — always send cultures | |||
*Blood cultures | |||
*[[CBC]], [[ESR]], [[CRP]] | |||
*Uric acid (may be normal during acute gout flare) | |||
*X-ray of affected joint | |||
===Polyarticular=== | |||
*[[CBC]], [[BMP]], [[ESR]], [[CRP]] | |||
*Rheumatoid factor, anti-CCP (rheumatoid arthritis) | |||
*ANA (SLE) | |||
*GC/CT NAAT, blood cultures if infectious etiology suspected | |||
*Hepatitis B/C, parvovirus B19 serologies if viral arthritis suspected | |||
*ASO titer if rheumatic fever suspected | |||
*X-rays of affected joints | |||
*Consider echocardiography if endocarditis suspected | |||
==Management== | |||
===Septic Arthritis=== | |||
*Emergent orthopedic consultation for drainage | |||
*Empiric IV antibiotics: [[vancomycin]] +/- [[ceftriaxone]] (see [[Septic arthritis]]) | |||
===Crystal Arthropathy=== | |||
*NSAIDs ([[indomethacin]], [[naproxen]]), [[colchicine]], or corticosteroids | |||
*Intra-articular steroid injection after ruling out infection | |||
*See [[Gout]], [[Pseudogout]] | |||
===Inflammatory/Autoimmune=== | |||
*NSAIDs for symptomatic relief | |||
*Rheumatology consultation/referral | |||
*Specific management depends on underlying diagnosis | |||
===Gonococcal Arthritis=== | |||
*[[Ceftriaxone]] + treat for chlamydia co-infection | |||
*See [[Gonococcal arthritis]] | |||
==Disposition== | |||
===Admit=== | |||
*Septic arthritis (for surgical drainage and IV antibiotics) | |||
*Prosthetic joint infection | |||
*Endocarditis | |||
*Severe systemic inflammatory process | |||
*New rheumatic fever | |||
===Discharge=== | |||
*Crystal arthropathy with adequate pain control | |||
*Viral arthritis | |||
*Known autoimmune arthritis with mild flare | |||
*Arrange rheumatology follow-up for new polyarthritis | |||
*Return precautions: fever, worsening joint swelling, new joint involvement, inability to bear weight | |||
==See Also== | |||
*[[Monoarticular arthritis]] | |||
*[[Septic arthritis]] | |||
*[[Arthrocentesis]] | |||
*[[Gout]] | |||
*[[Pseudogout]] | |||
*[[Rheumatoid arthritis]] | |||
*[[Gonococcal arthritis]] | |||
==External Links== | |||
==References== | |||
<references/> | |||
[[Category:Orthopedics]] | |||
[[Category:Rheumatology]] | |||
[[Category:Symptoms]] | |||
Latest revision as of 10:49, 22 March 2026
Background
- Arthritis refers to joint inflammation, characterized by pain, swelling, warmth, and decreased range of motion[1]
- The primary EM concern is ruling out septic arthritis, which is a joint emergency requiring urgent drainage
- Classification by number of joints involved helps narrow the differential:
- Monoarticular (1 joint): septic arthritis, crystal disease, hemarthrosis — see Monoarticular arthritis
- Oligoarticular (2-4 joints): reactive arthritis, seronegative spondyloarthropathy, gonococcal arthritis
- Polyarticular (≥5 joints): rheumatoid arthritis, viral arthritis, SLE, rheumatic fever
- Migratory: rheumatic fever, gonococcal arthritis, viral
- Key distinction: inflammatory (warm, swollen, worse with rest, morning stiffness >30 min) vs. non-inflammatory/mechanical (worse with activity, minimal swelling, no morning stiffness)
Clinical Features
History
- Number and pattern of joints involved
- Acute vs. chronic onset
- Symmetric vs. asymmetric distribution
- Morning stiffness: >30-60 minutes suggests inflammatory arthritis
- Recent infection: pharyngitis (post-strep/rheumatic fever), GI illness (reactive arthritis), STI (gonococcal)
- Skin findings: rash, psoriasis, tophi, dermatitis-arthritis syndrome
- Eye symptoms: conjunctivitis (reactive arthritis), uveitis (ankylosing spondylitis)
- Trauma history
- Family history of autoimmune disease
- Medication history: diuretics, cyclosporine (gout risk)
Physical Exam
- Joint warmth, swelling, effusion, tenderness
- Range of motion (active and passive)
- Pain with passive ROM suggests intra-articular pathology
- Periarticular tenderness without effusion suggests bursitis/tendinitis (periarticular, not articular)
- Skin: tophi (gout), dactylitis (psoriatic arthritis), rash, nail pitting (psoriasis)
- Mucocutaneous lesions (gonococcal — pustules on palms/soles, tenosynovitis)
- Heart murmur (endocarditis, rheumatic fever)
Red Flags
- Hot, swollen, single joint = septic until proven otherwise → arthrocentesis
- Fever with joint complaints (septic arthritis, endocarditis)
- Prosthetic joint with new pain/swelling (prosthetic joint infection)
- IV drug use + joint pain (hematogenous seeding)
- Polyarthritis + new murmur (endocarditis)
- Pediatric arthritis + fever + rash (consider Kawasaki disease, rheumatic fever, JIA)
Differential Diagnosis
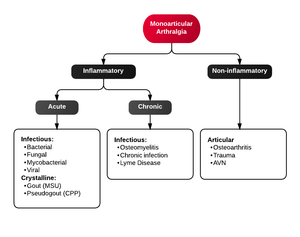
Monoarticular arthritis
- Acute osteoarthritis
- Avascular necrosis
- Crystal-induced (Gout, Pseudogout)
- Gonococcal arthritis, arthritis-dermatitis syndrome
- Nongonococcal septic arthritis
- Lyme disease
- Malignancy (metastases, osteochondroma, osteoid osteoma)
- Reactive poststreptococcal arthritis
- Trauma-induced arthritis
- Fracture
- Ligamentous injury
- Overuse
- Avascular necrosis
- Decompression sickness
- Spontaneous osteonecrosis
- Hemorrhagic (e.g. hemophilia, systemic anticoagulation
- Seronegative spondyloarthropathies (ankylosing spondylitis, IBD, psoriatic arthritis, reactive arthritis
- RA, SLE
- Sarcoidosis, amyloidosis
- Periarticular pathology
- Transient (Toxic) Synovitis (Hip)
- Slipped Capital Femoral Epiphysis (SCFE)
- Legg Calve Perthes Disease
Oligoarthritis
- Ankylosing spondylitis
- Gonococcal arthritis
- Lyme disease
- Psoriatic arthritis
- Reactive arthritis
- Rheumatic fever
- Rheumatoid arthritis
- Systemic lupus erythematosus
Polyarthritis
- Fibromyalgia
- Juvenile idiopathic arthritis
- Lyme disease
- Osteoarthritis
- Psoriatic arthritis
- Reactive poststreptococcal arthritis
- Rheumatoid arthritis
- Rheumatic fever
- Serum sickness
- Systemic lupus erythematosus
- Serum sickness–like reactions
- Viral arthritis
Migratory Arthritis
- Gonococcal arthritis
- Lyme disease
- Rheumatic fever
- Systemic lupus erythematosus
- Viral arthritis
Evaluation
Monoarticular (Most Critical Workup)
- Arthrocentesis — perform on any acute hot, swollen joint
- Synovial fluid: cell count, Gram stain, culture, crystal analysis
- WBC >50,000 with >90% PMNs = presumed septic until culture results
- Crystals: negatively birefringent (gout), positively birefringent (pseudogout)
- Note: crystals do NOT rule out co-existing infection — always send cultures
- Blood cultures
- CBC, ESR, CRP
- Uric acid (may be normal during acute gout flare)
- X-ray of affected joint
Polyarticular
- CBC, BMP, ESR, CRP
- Rheumatoid factor, anti-CCP (rheumatoid arthritis)
- ANA (SLE)
- GC/CT NAAT, blood cultures if infectious etiology suspected
- Hepatitis B/C, parvovirus B19 serologies if viral arthritis suspected
- ASO titer if rheumatic fever suspected
- X-rays of affected joints
- Consider echocardiography if endocarditis suspected
Management
Septic Arthritis
- Emergent orthopedic consultation for drainage
- Empiric IV antibiotics: vancomycin +/- ceftriaxone (see Septic arthritis)
Crystal Arthropathy
- NSAIDs (indomethacin, naproxen), colchicine, or corticosteroids
- Intra-articular steroid injection after ruling out infection
- See Gout, Pseudogout
Inflammatory/Autoimmune
- NSAIDs for symptomatic relief
- Rheumatology consultation/referral
- Specific management depends on underlying diagnosis
Gonococcal Arthritis
- Ceftriaxone + treat for chlamydia co-infection
- See Gonococcal arthritis
Disposition
Admit
- Septic arthritis (for surgical drainage and IV antibiotics)
- Prosthetic joint infection
- Endocarditis
- Severe systemic inflammatory process
- New rheumatic fever
Discharge
- Crystal arthropathy with adequate pain control
- Viral arthritis
- Known autoimmune arthritis with mild flare
- Arrange rheumatology follow-up for new polyarthritis
- Return precautions: fever, worsening joint swelling, new joint involvement, inability to bear weight
See Also
- Monoarticular arthritis
- Septic arthritis
- Arthrocentesis
- Gout
- Pseudogout
- Rheumatoid arthritis
- Gonococcal arthritis
External Links
References
- ↑ Ross JJ. Septic Arthritis of Native Joints. Infect Dis Clin North Am. 2017 Jun;31(2):203-218. PMID 28366221